

About Breast cancer
One in eight women develops Breast cancer during their lifetime, making it one of the most common cancers worldwide. Breast cancer can affect one or both breasts, which can occur in different parts of the breast, and it is an abnormal growth occurring in the breast that could spread. Almost entirely, these cases are found in women, but men can also develop Breast cancer.


Risk Factors & Prevention
Women ages 45 and older are at a higher risk of Breast cancer.
Some risk factors are:
- Increased Weight
- Alcohol Consumption
- Unhealthy Lifestyle & Diet
- Menstrual and Reproductive History
- Radiation exposure
- Late Pregnancy
- Gene Mutations
- Family History of Breast cancer
- Hormone Pills
How can it be prevented?
- Maintain a Healthy Weight
- Be Physically Fit & Maintain a Proper Diet
- Reduce Hormone Intake
- Limit Smoking & Drinking
- Avoid Birth Control Pills
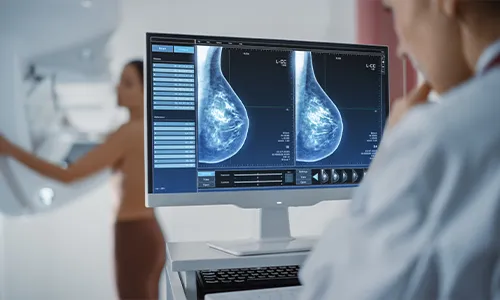

Screening
Screening exams for Breast cancer help detect cancer at an early stage.
The likelihood of successful treatment is increased by early diagnosis:
- Mammography
- Breast Ultrasound
- Magnetic Resonance imaging
- Clinical Breast Exams


Symptoms & Signs
- Usually there is a painless lump to begin with however there may be pain in the breast when a breast lump has grown to involve the overlying skin
- Perforated and swollen skin throughout the breast region
- Inflammation in different parts of the breast
- A nipple discharge that is unusual and just not breast milk
- Blood coming out of your nipple
- Skin that is flaky, peeling, or scaly on your nipple
- A sudden change in your breast size
- An upside-down nipple
- A change in the way your breast flesh looks
- A lump beneath your arm


Diagnosis
Breast cancer diagnostic tests determine whether you have the disease and how aggressive it may be.
Tools and tests include:
- Lab tests
- Biopsy
- MRI or Mammogram
- Staging Tests
- PET-CT


Sub-Type of Breast cancers and Stages
-
Non-Invasive Cancer
- Ductal Carcinoma in Situ (DCIS)
-
Invasive Cancer
- Invasive lobular carcinoma (ILC)
- Invasive ductal carcinoma (IDC)
- Angiosarcoma of the Breast
- Inflammatory Breast cancer
- Paget Disease of the Breast
- Phyllodes Tumors
Cancer has five Stages 0 through IV
Stage 0:
At this Stage, the disease is non-invasive, which indicates that it hasn’t broken out from breast ducts.
Stage 1:
The surrounding breast tissue has become infected with cancerous cells.
Stage 2:
The breast tumor is either smaller than 2 centimeters in diameter and spread to the lymph nodes under the arms or greater than 5 centimeters in diameter but hasn’t spread yet. At this Stage, breast tumors may or may not impact the adjacent lymph nodes.
Stage 3:
Cancer has already spread past its origin at this point and it might have spread to neighboring lymph nodes and tissue, but it hasn’t reached distant organs. Breast cancer at Stage III is typically referred to as locally advanced Breast cancer.
Stage 4:
Cancer at this Stage is called metastatic Breast cancer. Your brain, bones, liver, lungs, or other organs may also have been affected, in addition to your breast.


Treatment Modalities
a. Surgical Oncology
A few of the prominent surgical options for treating Breast cancer:
- Lumpectomy – Preserving the remainder of the breast while removing the breast tumor and the infected. Surrounding tissues.
- Mastectomy – Removing the entire breast or both the breasts.
- Sentinel node biopsy – Removing a few lymph nodes that are affected and are tested for cancerous cells.
- Axillary lymph node dissection – Removing additional lymph nodes if the Sentinel node biopsy lymph nodes are found to have malignancy.
- Contralateral prophylactic mastectomy – Removing the healthy breast to prevent cancer from occurring in that breast of a patient with BRCA gene mutation.
b. Medical Oncology
Chemotherapy is not always necessary for Breast cancer patients.
Your oncologist (cancer specialist) may advise chemotherapy depending on the Stage of the disease:
- Before surgery – Neoadjuvant chemotherapy to shrink the breast tumor size. It also allows healthcare providers to learn more about the biology of the disease resulting in less-extensive surgery.
- After surgery – Adjuvant chemotherapy is recommended by healthcare providers to kill any remaining cancer cells. Since malignant cells might occasionally still be present in your body despite not being detected by imaging tests. It also reduces the chances of cancer recurrence.
- For advanced cancer – Chemotherapy may be the primary treatment if your Breast cancer has metastasized (spread to other places of your body).
- For IBC – Inflammatory Breast cancer (IBC) does not typically have an easily – removable lump. The first course of action for IBC is chemotherapy.
c. Radiation Oncology
- Utilizes carefully regulated radiation beams to destroy cancer cells or relieve symptoms associated with cancer.


Coping with Treatment
Along with the medical side effects of Breast cancer therapy, patients also deal with the financial burden of cancer care and the emotional and social impacts. Talking to a counselor or family member can help them to cope with treatment. MOC provides facility of psycho Onco-Counseling and Nutritional counseling to help patients.


Do’s & Don’ts During Treatment
Do’s
- Maintain a healthy sleep schedule
- Be physically active
- Minimize attending public gatherings
- Yoga and meditation
- Maintain a decent, adequate, and nutritional diet regime
Dont’s
- Avoid Overexertion yourself
- Avoid an Unhealthy lifestyle
- Avoid getting exposed to Infections
- Avoid taking the stress
- Do not miss follow-up visits
- Avoid eating large meals
- Quit smoking, Alcohol


Post Treatment Support
Post-treatment Breast cancer survivors can undergo long-term side effects of surgery, radiation therapy, chemotherapy, and hormonal therapy. They can also have symptoms as Menopausal symptoms, such as hot flashes, Joint pain, Fatigue, Mood changes, Depression, and anxiety. Survivors require empathy, mental strength, and support from their families; they can also join Breast cancer Post-Treatment Survivorship Support Groups.


Follow-ups Cancer Care Plan
Post-treatment, one must request a follow-up treatment plan. Doctors provide a personalized treatment plan based on the type and Stage of cancer.


Surveillance and monitoring for indications of recurrence
One aim of follow-up care is checking for a recurrence. One should never miss follow-up visits and never ignore any symptoms of recurrence. Because some cancer cells may remain undiscovered in the body in small locations that don’t respond to treatment, cancer can reoccur. A physician knowledgeable about your medical history can provide personalized information regarding your risk of recurrence during follow-up care.


FAQ’s
-
Breast cancer? what is it?
Breast cancer is a type of cancer that develops in one or both breasts.
-
Who can get Breast cancer?
All women can be affected by Breast cancer; in some cases, men can also get Breast cancer.
-
What signs or symptoms does Breast cancer have?
A new breast tumor or lump is the most typical indication of Breast cancer. Breast cancers can be painful, soft, or circular, but they are more likely to be malignant if they are painless, firm, and have uneven borders.
-
Can Breast cancer be genetically inherited?
Yes, in 5-10% of cases, mutations can be inherited
-
How long do I need to wait to get pregnant after treatment for Breast cancer?
Some Breast cancer survivors are recommended to wait at least two years after their treatment is over before attempting pregnancy.
-
Is Breast cancer contagious?
No. One can’t catch cancer from some other person like flu or cold.
-
After Breast cancer therapy, can I breastfeed?
Breastfeeding difficulties from the afflicted breast could result after surgery, radiation, or both.
Specialized Doctors at M | O | C
Find the nearest center
Cancer Centres
Mumbai
Pune
Rest of Maharashtra
Gujarat
Delhi NCR
Cancer Clinics
Borivali
+91 9920767626
Explore More
-
Chemotherapy
Chemotherapy employs drugs to eradicate cancer cells. With this specific cancer therapy, cancer cells are prevented from multiplying, dividing, and generating new cells. A number of cancers can be treated using chemotherapy. Your doctor may refer to chemotherapy as normal chemotherapy, conventional chemotherapy, or cytotoxic chemotherapy. The medicine chemotherapy has an overall body-wide impact. This implies that it circulates throughout the body via the bloodstream. Chemotherapy comes in a variety of forms. Chemotherapy drugs, in general, are strong chemicals that destroy malignant cells at specific stages of the cell cycle. In all living things, new cells are produced by a process called the cell cycle. Chemotherapy has a greater effect on these rapidly multiplying cells because cancer cells go through this cycle faster than healthy cells.
Read more -
Immunotherapy
Immunotherapy, a wide term for a class of drugs used to treat cancer, activates the immune system to fight cancer cells. Healthy cells naturally die off, however, cancer cells do not. They proliferate like an untamed copy machine that won’t quit. The immune system, which protects the body from infections and disease, is unable to identify these abnormal cells because they frequently alter or mutate. In order for the immune system to detect and destroy these changed cells, drugs employed in cancer immunotherapy are designed to alert it to their presence. Immunotherapy is a treatment option for several types of cancer. It may be used alone or in conjunction with other cancer treatments such as chemotherapy.
Read more -
Targeted Therapy
Targeted therapy is a method of cancer treatment that identifies and kills specific cancer cell types. Targeted therapy may be used alone or in conjunction with other forms of therapy, including radiation therapy, surgery, conventional chemotherapy, and immunotherapy. Knowing how it functions and what to anticipate can frequently help you get ready for treatment and make wise decisions about your care if your treatment plan calls for targeted therapy. “Targeted therapy” for cancer focuses on particular proteins that control the growth, proliferation, and spread of cancer cells. Precision medicine is built on this principle. As information about the DNA alterations and proteins that feed cancer grows, researchers are better able to create cancer therapies that target these proteins.
Read more -
Palliative Care
Palliative care is a medical treatment designed to enhance the quality of life for people with serious or life-threatening illnesses, such as cancer. It may be administered with or without curative therapy. Along with cancer treatments that aim to stop, slow down or cure cancer, palliative care is a crucial component of medical therapy. Palliative care, according to research, can increase your quality of life and make you feel happier with your medical care. Palliative care may begin as soon as you find that you have cancer and you may continue to get it while undergoing treatment and recovering. For instance, palliative care may be provided to cancer survivors who continue to experience symptoms or side effects after their treatment has finished.
Read more -
2nd Opinion Clinic
A second opinion is a medical diagnosis offered by a medical professional or organization other than the one currently treating the patient. The patient or their family or friends give the second doctor access to the patient’s medical information. The second doctor evaluates the records and offers a Second Opinion on the best course of treatment, outlining why it is the best option. In complex circumstances, second opinions offer the chance to review the problem with a panel of experts or a tumor board and suggest the best, most patient-centered course of action. The patient is free to decide whether or not to accept an opinion of their own.
Read more
Book Your Appointment



























.png)









.png)




















.png)
.png)
.png)








