- About
- Risk Factors & Prevention
- Screening
- Symptoms & Signs
- Diagnosis
- Sub-Types and Stages
- Grading of Brain tumors
- Treatment Modalities
- Coping with Treatment
- Do’s & Don’ts During Treatment
- Post-Treatment Support
- Follow-ups Cancer Care Plan
- Surveillance and monitoring for Signs & Symptoms of Recurrence
- FAQ's


About Brain Cancer
In place of brain cancer, clinicians frequently refer to brain tumors. The majority of brain tumors can spread via the brain tissue, but they seldom do so to other regions of the body. Even so-called benign brain tumors have the potential to cause catastrophic or even life-threatening damage when they advance and obliterate healthy brain tissue. Brain tumors can alter a person’s thinking, speech, or movement patterns.


Risk Factors & Prevention
Men are more likely than women to get a brain tumor. Meningioma is one particular type of brain tumor that is more frequent in women.
Some risk factors are:
- Exposure to radiation
- Family history
- Exposure to electromagnetic radiation from power lines and transformers and a compromised immune system
- Occupational exposure to pesticides and herbicides
- Head Injury
- Exposure to viruses, bacteria, and allergens
How can it be prevented?
Unfortunately, brain tumors cannot be prevented. By avoiding exposure to radiation to the brain and staying away from environmental dangers like smoking, one can lower their risk of acquiring a brain tumor.


Screening
There aren’t any tests that are frequently advised right now to check for malignancies in the brain and spinal cord. The majority of brain tumors are discovered when a patient visits the doctor due to indications or symptoms they are experiencing.


Symptoms & Signs
- Headaches that could be really bad and get worse during physical exercise or in the morning
- Seizures can take many distinct forms
- Myoclonic- Muscle jerks, twitches, or spasms in one or more muscles
- Tonic-Clonic (Grand Mal)- Loss of awareness and body tonality, followed by contractions – the twitching and relaxing of muscles
- Sensational, visual, auditory, and/or olfactory changes without loss of consciousness
- Partial Seizures may result in a loss of consciousness, including total or partial loss of awareness or may be connected to inadvertent, recurrent twitching motions
- Changes in personality or memory
- nausea or vomiting
- Fatigue
- Drowsiness
- issues with sleep
- alterations in one’s capacity to move or carry out daily tasks
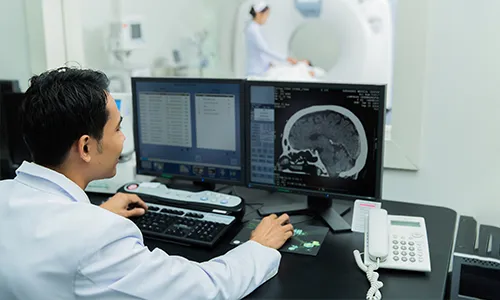

Diagnosis
Brain cancer diagnostic tests determine whether you have the disease and how aggressive it may be.
Tools and tests include:
- Biopsy
- MRI
- PET-CT scan
- Electroencephalography (EEG)
- Neurological, vision, and hearing tests
- Biomarker
- Myelogram
- Lumbar puncture
- Cerebral arteriogram


Sub-Types and Stages
-
Gliomas
- Astrocytoma
- Oligodendroglioma
- Ependymomas
-
Non-glioma tumors
- Meningioma
- Pineal gland and pituitary gland tumors
- Primary CNS lymphoma
- Embryonal tumors
- Medulloblastoma
- Schwannoma
- Germ cell tumors

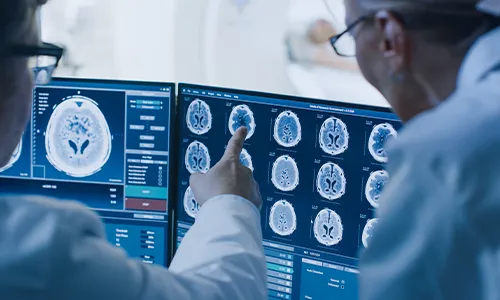
Grading of Brain tumors
Every type of brain cancer has a unique grading system:
Grade I:
At this stage the tumor is benign. The cells resemble brain tissue in almost every way. This is the least threatening grade.
Grade II:
The growth is cancerous. Although they are typically slow-growing cells, the cells appear more aberrant.
Grade III:
This malignant tumor has cells that have an incredibly aberrant appearance and are rapidly developing (anaplastic).
Grade IV:
The malignant tissue has cells with the most atypical appearance and a propensity to expand quickly.

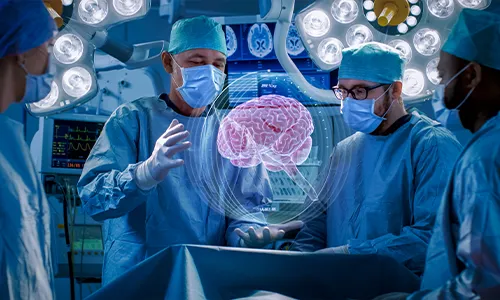
Treatment Modalities
a. Surgical Oncology
- The first course of treatment for a brain tumor is typically surgery. A surgeon who focuses on performing operations on the brain and spinal column is known as a neurosurgeon. Craniotomy is necessary for brain surgery, in this procedure a portion of the skull is removed.
- There have been significant improvements in brain tumor surgery, including the use of fluorescent dyes, improved imaging, and cortical mapping.
b. Medical Oncology
- Chemotherapy- Chemotherapy kills cancer cells by using chemicals. One chemotherapy medicine may be administered, or two or more drugs may be combined.
- Targeted Therapy- Targeted medication therapy may be used in conjunction with chemotherapy.
c. Electric field therapy
- The processes of a cell required for tumor cells to grow, develop and spread are interfered with using a noninvasive, portable device in this sort of treatment. It is supplied by attaching electrodes to a person’s head that create an electric field.
- Optune is the name of the accessible device, for those who have just received a glioblastoma diagnosis or for those who have recurrent glioblastoma.
d. Radiation Oncology
- Radiation therapy is one method that doctors may employ to delay or prevent the development of a brain tumor. There are several techniques to apply external-beam radiation therapy to a brain tumor as Conventional radiation therapy, 3-dimensional conformal radiation therapy (3D-CRT), Intensity-modulated radiation therapy (IMRT), proton therapy, stereotactic radiosurgery, and fractionated stereotactic radiation therapy.


Coping with Treatment
Along with the medical side effects of brain cancer therapy, patients also deal with the financial burden of cancer care and the emotional and social impacts. Talking to a counselor, or family member can help them to cope with treatment. MOC provides facility of psycho Onco-Counseling and Nutritional counseling to help patients.


Do’s & Don’ts During Treatment
Do’s
- Eat wholesome food
- Focus on having more food than multivitamins
- Maintain an optimum weight
Don’ts
- Avoid Overexertion
- Avoid an unhealthy lifestyle
- Avoid taking stress


Post-Treatment Support
Post-treatment brain cancer survivors can go through long-term side effects of surgery, radiation therapy and chemotherapy. They can also have symptoms such as headaches, hair loss, nausea, vomiting, extreme tiredness (fatigue), infertility, hearing loss, and cataracts. Survivors require empathy, mental strength, and support from their families, they can also join brain cancer Post-Treatment Survivorship Support Groups.


Follow-ups Cancer Care Plan
Post-treatment one must request a follow-up treatment plan. Doctors provide a personalized treatment plan based on the type and stage of cancer.


Surveillance and monitoring for Signs & Symptoms of Recurrence
One aim of follow-up care is checking for a recurrence. One should never miss follow-up visits and never ignore any symptoms of recurrence. Because some cancer cells may remain undiscovered in the body in small locations that don’t respond to treatment, cancer can reoccur. A physician who is knowledgeable about your medical history can provide you with personalized information regarding your risk of recurrence during follow-up care


FAQs
-
What Are the Complications of Surgery for Brain Cancer?
Bleeding in the brain, brain swelling, infection, a reaction to the anesthetic drug, blood clots, impaired motor or memory functions, seizures
-
Things to be aware of regarding a brain tumor?
Each tumor has a distinct cellular composition, there are two types of brain tumors: primary and secondary. You could have more options for treatment than you realize.
-
Three Signs of a Brain Tumor You Should Not Ignore?
Seizures, a lack of ability to communicate or react to speech, unexpected onset of vision haze and a persistent headache.
Specialized Doctors at M | O | C
Find the nearest center
Cancer Centres
Mumbai
Pune
Rest of Maharashtra
Gujarat
Delhi NCR
Cancer Clinics
Borivali
+91 9920767626
Book Your Appointment



























.png)









.png)




















.png)
.png)
.png)







