

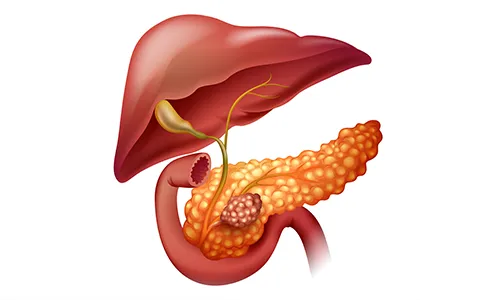
About Pancreatic Cancer
In pancreatic cancer, healthy cells in the pancreas begin to malfunction and proliferate out of control. These malignant cells can aggregate and develop into a mass known as a tumor. Malignant refers to the ability of a cancerous tumor to develop and metastasize to different body regions.


Risk Factors & Prevention
Adults over 45 are most likely to get pancreatic cancer. Some of the risk factors:
- Obesity
- Smoking
- Diabetes
- Family History
- Rare inherited conditions
- Exposure to chemicals
- Liver Cirrhosis
- Infections and bacteria
How can it be prevented?
- Quit Smoking
- Maintain healthy weight
- Avoid Alcohol
- Limit exposure to chemicals

Screening
Finding pancreatic cancer early is challenging. Early tumors cannot be seen or felt by healthcare professionals during standard physical exams since the pancreas is located deep inside the body. Some persons may have a higher chance of developing pancreatic cancer due to family history. Genetic testing searches for the gene alterations that result in these inherited disorders and raise the risk of pancreatic cancer.


Symptoms & Signs
- Yellow skin and/or eyes, darkened urine, itching, and feces that is the color of clay
- Upper abdominal, upper back, or arm pain
- A painful blood clot-related swelling of the arm or leg
- Various gastrointestinal discomforts such as a burning sensation in the stomach
- Abdominal bloating
- Stools that float and have an odd color and smell because the body is having trouble processing fats
- Weakness
- The inability to eat
- Nausea and diarrhea
- Sweats and chills
- Fever
- Unaccounted-for weight loss

Diagnosis
Pancreatic cancer diagnostic tests determine whether you have the disease and how aggressive it may be.
Tools and tests include:
- Physical examination
- Blood tests
- CA19-9
- Imaging tests
- CT or CAT scan
- PET-CT scan
- Endoscopic retrograde cholangiopancreatography (ERCP)
- Ultrasound
- Transabdominal ultrasound
- The endoscopic ultrasound (EUS)
- PTC
- MRI
- Biopsy
- Fine needle aspiration (FNA)
- Core needle biopsy
- biomarker

Sub-Types and Stages
- Exocrine tumors
- Ductal adenocarcinoma
- Intraductal papillary mucinous neoplasm (IPMN)
- Acinar cell carcinoma
- Adenosquamous carcinoma
- Colloid carcinoma
- Giant cell tumor
- Hepatoid carcinoma
- Mucinous cystic neoplasms
- Pancreatoblastoma
- Serous cystadenoma
- Signet ring cell carcinoma
- Solid and pseudopapillary tumors
- Squamous cell carcinoma
- Undifferentiated carcinoma
- Endocrine tumors
- Pancreatic neuroendocrine tumors (PNETs)
Stages
Stage 0:
Describes cancer in situ, which has not yet spread outside of the duct in which it first appeared.
Stage 1:
A pancreatic tumor with a diameter of 2 cm or less. The lymph nodes are not affected.
Stage 2:
The tumor is above 4 cm in size and has spread outside the pancreas. It has not migrated to neighboring lymph nodes, arteries, veins, or other body organs.
Stage 3:
Any size tumor that has reached four or more local lymph nodes but not the arteries, veins, or other bodily organs in the area.
Stage 4:
Tumor that has progressed to other bodily parts.


Treatment Modalities
a. Surgical Oncology
- Surgery for pancreatic cancer could require removing all or a portion of the pancreas, based on the location and severity of the pancreatic tumor. A piece of the tumor’s surrounding healthy tissue is frequently removed as well. Depending on the surgery’s goal, various surgical procedures are carried out laparoscopy, whipple procedure, distal pancreatectomy, and total pancreatectomy.
b. Medical Oncology
- Chemotherapy- Chemotherapy kills cancer cells by using chemicals. One chemotherapy medicine may be administered, or two or more drugs may be combined.
- Targeted Therapy- For the treatment of advanced endometrial cancer, targeted medication therapy is frequently used in conjunction with chemotherapy.
- Immunotherapy- A medicinal therapy called immunotherapy supports the immune system’s ability to fight cancer. If the cancer is advanced and other treatments have failed for endometrial cancer, immunotherapy may be tried.
c. Radiation Oncology
- To kill cancer cells, radiation therapy employs powerful energy beams like protons and X-rays. Radiation from a machine outside of your body or radiation implanted inside of your body can both be used in radiation therapy.


Coping with Treatment
Along with the medical side effects of pancreatic cancer therapy, patients also deal with the financial burden of cancer care and the emotional and social impacts. Talking to a counselor, or family member can help them to cope with treatment. MOC provides facility of psycho Onco-Counseling and Nutritional counseling to help patients.


Do’s & Don’ts During Treatments
Do’s
- Maintain healthy weight
- Keep yourself hydrated
- Eat small meals
Don’ts
- Reduce sugar intake
- Avoid red meat
- Reduce caffeine and alcohol intake


Post-Treatment Support
Post-treatment pancreatic cancer survivors can go through long-term side effects of surgery, radiation therapy, chemotherapy, and hormonal therapy. They can also have symptoms such as extreme tiredness (fatigue), diarrhea, being sick, loss of appetite, taste changes or a sore mouth, losing hair, numbness in your fingers or toes, and blood clots. Survivors require empathy, mental strength, and support from their families, they can also join pancreatic cancer Post-Treatment Survivorship Support Groups.


Follow-ups Cancer Care Plan
Post-treatment one must request a follow-up treatment plan. Doctors provide a personalized treatment plan based on the type and stage of cancer.


Surveillance and monitoring for Signs & Symptoms of Recurrence
One aim of follow-up care is checking for a recurrence. One should never miss follow-up visits and never ignore any symptoms of recurrence. Because some cancer cells may remain undiscovered in the body in small locations that don’t respond to treatment, cancer can reoccur. A physician who is knowledgeable about your medical history can provide you with personalized information regarding your risk of recurrence during follow-up care


FAQ’s
-
Which factors lead to pancreatic cancer?
Fundamentally, DNA damage is what causes pancreatic cancer. These DNA changes can develop in one of three ways: either through inheritance, by actions like smoking, or just by chance.
-
What Can I Do to Lower My Chances of Pancreatic Cancer?
One should think about quitting smoking, losing weight, considering genetic testing, or taking part in screening trials for early cancer detection if pancreas cancer runs in your family.
-
Who is at the highest risk?
People whose family has at least two cases of pancreatic cancer. Ashkenazi Jewish people, those who smoke, are over 50 years old, and overweight people.
Specialized Doctors at M | O | C
Find the nearest center
Cancer Centres
Mumbai
Pune
Rest of Maharashtra
Gujarat
Delhi NCR
Cancer Clinics
Borivali
+91 9920767626
Book Your Appointment




























.png)









.png)




















.png)
.png)
.png)









