
About Cervical Cancer
The first sign of cervical cancer is when the human papillomavirus (HPV) infection or a change in healthy cells on the surface of the cervix triggers the development of a lump. A growth or tumor on the cervix can develop as a result of a long-term HPV infection that has affected the cervix.


Risk Factors & Prevention
Others with no known risk factors for cancer develop it, despite the fact that some people with a number of risk factors never do.
The following factors may increase the chance of developing cervical cancer:
- Human papillomavirus (HPV) infection
- Deficiency in the Immune system
- Genital Herpes
- Use of tobacco/smoking
- Use of Oral contraceptives
- Multiple sexual partners
- Diethylstilbestrol (DES) exposure
How can it be prevented?
- Quit smoking
- Putting off until the late teens or later for the first sexual intercourse
- Minimalizing the number of sexual partners
- Use dental dams and condoms to engage in safer sex
- Avoid having sex with someone who has been in several relationships
- Avoiding sexual activity with those who have genital warts or exhibit other signs


Screening
Screening exams for cervical cancer help detect cancer at an early Stage.
The likelihood of successful treatment is increased by early diagnosis:
- HPV test
- Pap test
- Visual inspection with acetic acid (VIA)


Symptoms & Signs
- Very mild bleeding or blood spots before or after periods
- Longer and heavier than usual menstrual bleeding
- Bleeding after sex or a pelvic examination
- Abnormal vaginal discharge
- Having painful sexual intercourse
- Following menopause, bleeding
- Persistent, irrational back and/or pelvic discomfort


Diagnosis
Cervical cancer diagnostic tests determine whether you have the disease and how aggressive it may be.
Tools and tests include:
- Bimanual pelvic examination and sterile speculum examination
- Pap test
- HPV typing test
- Colposcopy
- Biopsy
- Pelvic examination under anesthesia
- X-ray
- CT or CAT scan
- MRI
- PET-CT scan
- Biomarker
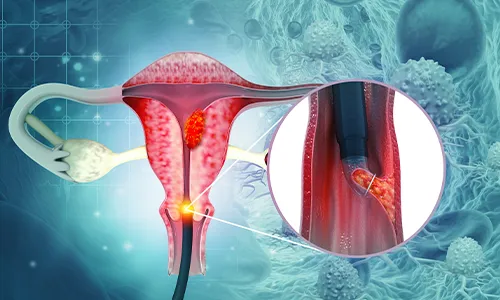

Sub-Types and Stages
- Squamous cell carcinoma
- Adenocarcinoma
Stages
Stage 1:
Cancer has only been diagnosed in the uterus but has spread from the lining of the cervix into deeper tissue.
Stage 2:
The cancer is still located inside the pelvic region, but it has migrated to neighboring tissues such as the vagina or tissue close to the cervix.
Stage 3:
The tumor affects the bottom part of the vagina and/or has migrated to the pelvic wall, producing hydronephrosis, swelling of the kidney, rendering one kidney inoperable, and/or involving local lymph nodes.
Stage 4:
Cancer has gone to the rectum or bladder, among other organs.


Treatment Modalities
a. Surgical Oncology
A few of the prominent surgical options for treating Cervical cancer:
- Conization- The procedure to remove all abnormal micro-invasive cancer tissue.
- Loop electrosurgical excision procedure (LEEP) – Procedure to remove micro-invasive cervical cancer tissue.
- Hysterectomy-Procedure to remove the uterus and cervix.
- Radical trachelectomy- Procedure to remove the cervix, but not the uterus.
- Exenteration- The removal of the uterus, vagina, lower intestine, rectum, or bladder if cervical cancer has progressed to these organs.
b. Medical Oncology
Chemotherapy is not always necessary for women with cervical cancer, although in some cases, it may be advised:
- Concurrent chemoradiation- The preferred course of treatment for various cervical cancer stages is concurrent radiation and chemotherapy.
- Advanced or recurrent cervical cancer- Cervical cancer that has spread to other organs and tissues may be treated with chemotherapy. When cervical cancer returns after receiving chemoradiation treatment, chemotherapy is most commonly advised.
c. Radiation Oncology
- Radiation therapy is used as part of the primary treatment or to treat cervical cancer that has spread or has returned after treatment, depending on the stage of the disease.


Coping with Treatment
Along with the medical side effects of cervical cancer therapy, patients also deal with the financial burden of cancer care and the emotional and social impacts. Talking to a counselor or family member can help them to cope with treatment. MOC provides facility of psycho Onco-Counseling and Nutritional counseling to help patients.


Do’s & Don’ts During Treatment
Do’s
- Maintain a healthy, nutritious diet
- Exercising daily
- Be in contact with emotional support groups
Don’ts
- Don’t miss follow-up visits
- Avoid processed meats


Post-Treatment Support
Post-treatment Cervical cancer survivors can undergo long-term side effects of surgery, radiation therapy, chemotherapy, and hormonal therapy. They can also have symptoms as Menopausal symptoms, such as hot flashes, Joint pain, Fatigue, Mood changes, Depression and anxiety. Survivors require empathy, mental strength, and support from their families, and they can also join Breast cancer Post-Treatment Survivorship Support Groups.


Follow-ups Cancer Care Plan
Post-treatment, one must request a follow-up treatment plan. Doctors provide a personalized treatment plan based on the type and stage of cancer.

Surveillance and monitoring for Signs & Symptoms of Recurrence
One aim of follow-up care is checking for a recurrence. One should never miss follow-up visits and never ignore any symptoms of recurrence. Because some cancer cells may remain undiscovered in the body in small locations that don’t respond to treatment, cancer can reoccur. A physician who is knowledgeable about your medical history can provide you with personalized information regarding your risk of recurrence during follow-up care.


FAQ’s
-
Cervical cancer: What is it?
Cancer that develops in a woman’s cervix is called cervical cancer.
-
Which signs and symptoms accompany cervical cancer?
Massive amounts of vaginal bleeding or discharge, bleeding following intercourse, during menstruation, or following a pelvic exam, and pain when urinating or having sex.
-
Who is prone to cervical cancer?
Cervical cancer is a risk for all women. Women above the age of 30 are at a higher risk of developing cervical cancer.
Specialized Doctors at M | O | C
Find the nearest center
Cancer Centres
Mumbai
Pune
Rest of Maharashtra
Gujarat
Delhi NCR
Cancer Clinics
Borivali
+91 9920767626
Book Your Appointment


























.png)









.png)




















.png)
.png)
.png)









